Scans and Services
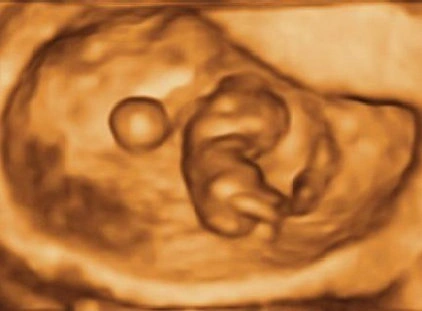
Dating Scan
Your Doctor may request this scan if you are unsure about your dates, you have bleeding or pain or if your doctor suspects a multiple pregnancy. The scan may also be performed if there is a history of ectopic pregnancies or recurrent miscarriage. Due to the small size of the baby at this early stage a transvaginal scan is normally performed. A transabdominal probe may also be used.
This scan will provide you with the following information:
1. The number of embryos and the pregnancy location. This can rule out an ectopic pregnancy.
2. The baby's heat rate. (This is usually present by 6 weeks)
3. The size of the embryo which will help to determine pregnancy dates. This is accurate to ± 3 days between 7 and 11 weeks. After 11 weeks the accuracy drops to ± 7 days because the baby curls up into the fetal position. We will also check for the presence of uterine fibroids or ovarian cysts.
The images provided by this scan are quite varied because the baby is growing so rapidly.
Less than 5 weeks: pregnancy is unlikely to be detected by scanning
5 – 6 weeks: A small gestation sac is seen
6 – 8 weeks: A small embryo around 5 mm is seen at 6 weeks
9 – 10 weeks: Limbs begin to develop
11 – 12 weeks: Baby curls up into fetal position
Dating scans may be done after 12 weeks if the nuchal has not been done and it is too early for a morphology scan
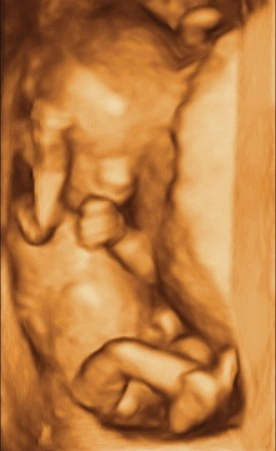
Nuchal Traslucency and/or Early Morphology
This test is done between 12weeks 4 days and 13weeks and 5 days by a Transabdominal scan.
The scan begins with an Early Morphology scan which looks at the heart, brain and other physical features of the baby.
The first trimeser nuchal translucency is a screening programme to find out your chance of having a baby with a major chromosomal abnormalities such as Down's Syndrome . Your doctor may have ordered a NIPT or Harmony test and may not request this part of the test to be done
The test has 2 parts;
1. An ultrasound measures the depth of fluid at the baby's neck called the nuchal translucency. (pronounced as 'new-cal').
2. A special blood test that measures the levels of two hormones- free beta HCG and PAAP-A. The blood test can be done between 10 - 14 weeks. The blood test poses no risk to the baby but you do have to have a needle. We will send you a blood form if you do not have one already. To receive this we will ask you to send a request to info@taraimaging.com.au so we can email it back to you.
At Tara we request that you have the blood test done at least 3 to 4 days before the scan. If you have the blood test done a few days before your scan we should be able to give you your final risk figure after the scan.
The doctor will speak to you personally about your risk and what the numbers mean. If the test places the pregnancy at a high risk of Down's Syndrome you may choose to do more invasive tests to determine if the baby has the condition.

Morphology 19-21 weeks
The morphology scan is the most detailed pregnancy scan done at Tara and we consider it one of the most important pregnancy scans.
It is done by a Transabdominal scan.
The baby will be thoroughly examined from its head to its toes and inside to outside to assess the baby's anatomy. This test gives a good indication of how your baby is physically developing. This is the test that will tell you if everything is progressing normally.
All the body will be looked at.
Toes and fingers counted, nose and lips examined, length of arms and legs, size of body and internal organs. The scan is looking to see if everything looks normal.
The heart rate will also be checked.
Normally most physical problems are showing some signs that can be detected at this stage of development. Many things can be corrected if detected early either before birth or shortly after birth. Either way it is better to be forewarned and prepared.
An ultrasound scan cannot detect conditions like Cerebral Palsy and Autism which have no physical signs.
If there is a problem the doctor will discuss it with you in detail after the scan and followup will be arranged.

Growth scan 24-42 weeks
Your doctor may request a growth scan for a number of reasons such as questions about the baby being large or small, the location of the placenta or as part of monitoring the pregnancy because of an underlying medical condition or past history.
Many things can be monitored if detected early and corrected shortly after birth. The scan will measure your baby and check the internal organs.
The pictures produce by this scan will reduce in quality after about 32 to 34 weeks due to there being a reduced gap between the uterine or placental wall and the baby. If the head is firmly planted against the wall we will not be able to get a picture of the face.
Information Provided
The size of the baby compared to dates.
The growth of the baby over time when data from previous scans is available.
The location of the placenta and if it is covering the cervix and if the cervix itself is closed. The size of the cervix cannot be determined in late pregnancy
The current presentation of the baby (e.g. breech).
Occasionally a problem will be detected by this scan that was not seen previously. The Doctor will discuss this with you in detail and organise followup if required.
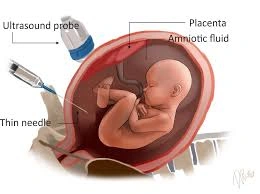
Amniocentesis
This procedure takes a sample of the amniotic fluid with a needle. The fluid contains some cells from the baby that are floating in the fluid and these are sent off for testing.
The needle does not touch the baby.
The sample will be sent by courier and usually is delivered the same day as the procedure. If you wish the rapid FISH test there will be an additional cost from the pathologist. The final results take around 2 weeks.
There is a small chance the sample may not contain enough of the baby's cells and the test may need to be repeated. This is rare.
This procedure can be done between 15 -18 weeks and has a 1 in 200 chance of miscarriage. You will be counselled by our Doctor before you have the test in order to make sure you understand the risks.
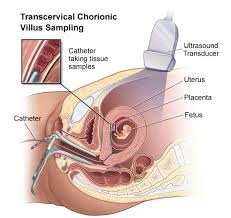
CVS
This procedure is similar to Amniocentesis except the sample is taken from the placenta instead of the amniotic fluid by either A (through the abdomen) or B (like a pap smear) depending on which is best in your case.
This test can be done between 11 to 13.5 weeks which is earlier than Amniocentesis. There is a small chance that the sample will not contain enough of the baby's cells and the test may need to be repeated. This is uncommon.
This procedure has a 1 in 100 chance of miscarriage. You will be counselled by our Doctor before you have the test in order to make sure you understand the risks.
It can tell you ;
The number and type of chromosomes present.
Any chromosomal abnormalities such as Down's syndrome.
The sex of the baby
This test cannot find all genetic conditions only major chromosomal abnormalities

AFI and Dopplers
Doppler studies use the same principle that police speed radar guns operate on. It is able to detect the speed and direction of movement. This is expressed as red and blue colours on the scan.
This is useful in measuring blood flowing in the placenta, umbilical artery and baby's heart.
These figures are then compared against the normal values to make sure all is progressing well.
If there is a problem it is not unusual to have this scan every few days.
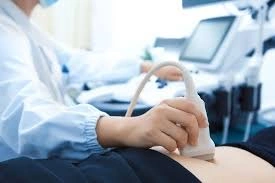
Pelvic
It is quite normal for you to be anxious or worried about a pelvic scan.
The procedure itself is usually not uncomfortable but often you are concerned about what it might find. Our job is to provide you with a quality scan done very gently with your privacy respected.
A pelvic scan is also done routinely before a Sonohysterogram or HYCOSY to exclude other problems and provide more information for an accurate report.
A pelvic scan is usually done both transabdominally and transvaginally. This is necessary to get the all the information required. 3D/4D scan is performed if an endometrial polyp or fibroid is suspected to assess the shape of the cavity and to check for the presence of an IUD (Intra-uterine device)
We do not do transvaginal scans without your consent or on children.
We do a very thourough scan that is examined by a Specialist Gynaecologist you can be confident that if something is present we will find it.
This means if your scan is normal your Doctor can confidently rule out a lot of possibilities. This also means expensive surgery or more invasive investigations can be avoided.
The Obstetrician and Gynaecologist will talk to you immediately and discuss the findings in detail to ensure you understand the scan results.
A pelvic ultrasound is done to check a woman's reproductive organs, the uterus and ovaries. Normal fallopian tubes are not usually seen on ultrasound.
The scan can be done for women of all ages to investigate any one of these conditions.
o Pelvic/period pain
o Heavy, painful, irregular or infrequent periods
o Postmenopausal bleeding
o Fertility workup
o Followup of a known ovarian cyst or mass
o To check ovaries
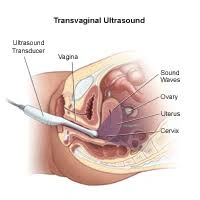
Deep Infiltrating Endometriosis Scan
This is a pelvic scan that looks for deep endometriosis. It cannot always detect superficial endometriosis.
This scan is best done with an empty bowel so you will need to take a mild laxative and fast on the day of the scan.
Deep infiltrating endometriosis is a relatively common source of pelvic pain in women and is important to exclude as a cause.
Transvaginal ultrasound is required for diagnosis with this scan.
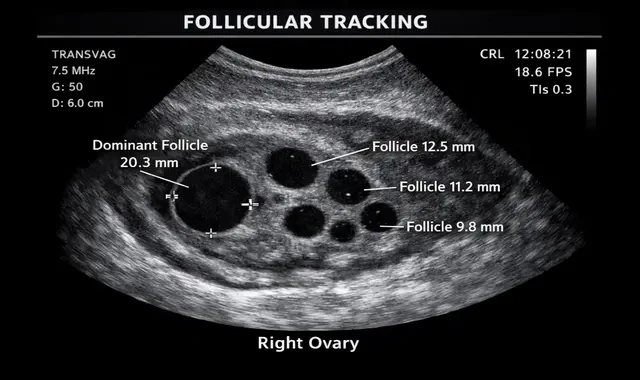
Fertility studies
Tara specialises in gynaecological scanning. We can provide information for you about uterine, ovarian and tubal causes of sub-fertility and infertility.
Endometriosis and polycystic ovaries are two of the most common causes of subfertility.
A pelvic scan can detect evidence of endometriosis by the presence of endometriomas within the ovaries.
Polycystic ovaries are also easily identified during transvaginal scanning and may be the cause of irregular periods and lack of ovulation.
We also can do a HYCOSY and Sonohysterogram to assess tubal patency and the uterine cavity
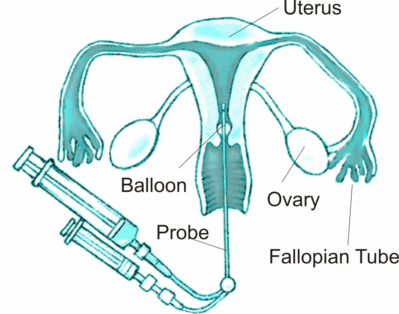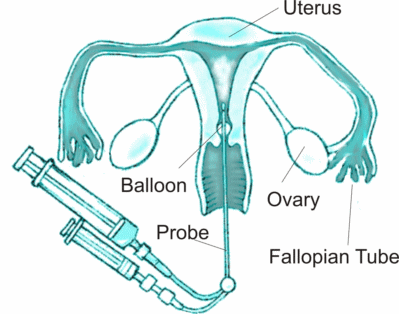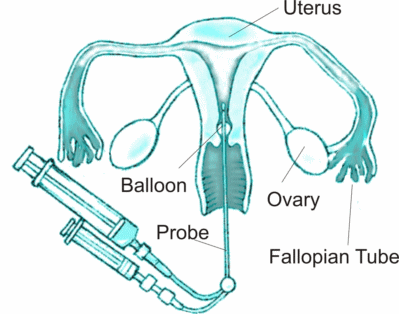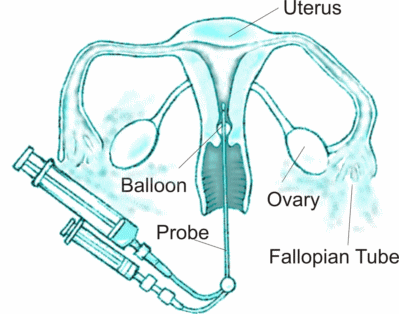
Hycosy
HYCOSY is a method of assessing if the fallopian tubes are blocked using ultrasound and levovist as contrast agent that makes the tubes stand out on ultrasound examination.
Hycosy is done as an investigation to assess fertility. 10 out of 100 couples experience difficulty conceiving a pregnancy. 3 /10 couples may be having these problems due to blockage of the fallopian tubes. Hycosy is a simple out-pateint procedure that can assess if the tubes are open.
The best time for the procedure is just after your period has finished and before ovulation, usually day 5 to day 10 of your cycle. This ensures that the procedure does not interfere with a possible early pregnancy.
You can eat and drink normally. Take 2 naprogesic tablets one hour before the procedure and drink 2 glasses of water. Naprogesics work best for pelvic pain.
The procedure itself takes a few minutes . We do advise that you allow at least 45 min to 1 hour from the time you come in to the time you leave.
The initial part of the procedure involves insertion of a vaginal ultrasound probe to image uterus and ovaries. After this is completed a vaginal speculum is inserted to see the cervix. The cervix is rinsed with an antiseptic solution. A sterile plastic catheter with a balloon at the end is inserted in the uterus. The balloon is then inflated gently to form a seal so that the dye does not come out of the uterus. Sterile solution is instilled into the cavity while the vaginal probe is used to scan the pelvis. The solution makes bright bubbles which make the tubes stand out on ultrasound. This is essentially the same as a Sonohysterogram except the special contrast agent is used.
The procedure is not usually painful however some women describe it as being uncomfortable or having mild cramping. The naprogesic tablets that are taken 1 hour before the procedure help in decreasing the discomfort.
Some women can feel faint after the procedure. This is a side effect of having a catheter dilate the cervix and will settle with 10 - 20 minutes of rest. There may be some spotting as a plastic catheter has been inserted into the lining of the uterus. The most serious complication is the risk of infection that occurs in less than 1% of women usually when there is a history of pelvic infection in the past. We encourage you to talk to your doctor who may advise you to have some antibiotics prior to the procedure.
Most women are able to drive after the procedure. However you may have discomfort or cramps during the procedure and it is best if you come with a support person who can drive you after the procedure.
Sonohysterogram
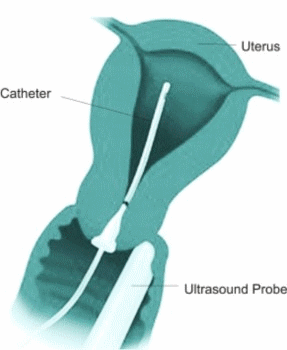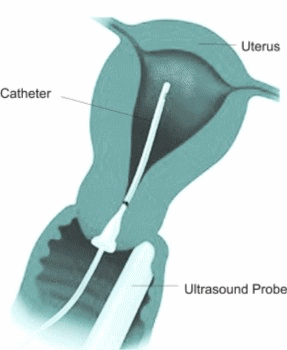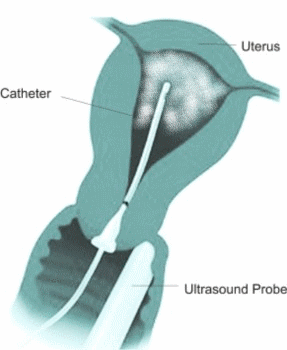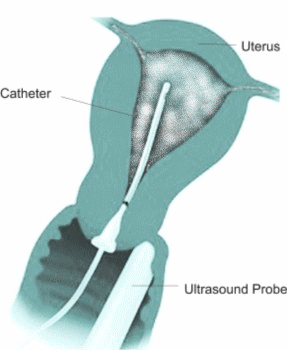
Sonohysterogram is a procedure in which a small amount of sterile saline is injected in the uterine cavity. The saline provides a black background against which abnormalities in the uterine cavity can be seen clearly on ultrasound.
Sonohysterogram is a method of assessing the endometrium and the shape of the cavity. It is commonly performed when the lining of the uterus is thickened, for suspected polyps and women on Tamoxifen. It is also used to assess uterine abnormalitys like bicornuate or septate uterus in women with history of recurrent miscarriages or premature delivery.
The best time for the procedure is just after your period has finished and before ovulation usually day 5 to day 10 of your cycle. This ensures that the procedure does not interfere with a possible early pregnancy.
You can eat and drink normally. Take 2 naprogesic tablets one hour before the procedure and drink 2 glasses of water. Naprogesics work best for pelvic pain.
The procedure itself takes a few minutes . We do advise that you allow at least 45 min to 1 hour from the time you come in to the time you leave.
The Doctor will insert a sterile vaginal speculum. This is similar to having a Pap smear. This allows uthe doctor to see your cervix and insert a sterile flexible soft tube into the uterus. The cervix is rinsed with an antiseptic solution before the insertion of the catheter. A plastic stopper is gently put at the end of the cervix to stop the saline water flowing back out. The speculum is then removed and the vaginal ultrasound probe is inserted in the vagina to capture images while the sterile saline is gently instilled into the uterine cavity. Once the imaging is completed both the cather and the probe are taken out at the same time. You may need to wear a pad after the procedure as some water may continue to drain.
The procedure is not usually painful however some women describe it as being uncomfortable or having mild cramping. The naprogesic tablets that are taken 1 hour before the procedure help in decreasing the discomfort.
Some women can feel faint after the procedure. This is a side effect of having a cather dilate the cervix and will settle with 10 -20 mins of rest. There may be some spotting as a plastic catheter has been inserted into the lining of the uterus. The most serious complication is the risk of infection that occurs in less than 1% of women usually when there is a history of pelvic infection in the past. We encourage you to talk to your doctor who may advise you to have some antibiotics prior to the procedure.
Most women are able to drive after the procedure. However you may have discomfort or cramps during the procedure and it is best if you come with a support person who can drive you after the procedure